Michael Joe Cini
22nd September 2022
Arthritis Management: Patients Take the Lead
“It’s about the patients becoming empowered to look after their own condition and be involved in that process” Dr David Gibson
BloodTrackR: Involving Patients in Arthritis Management Process
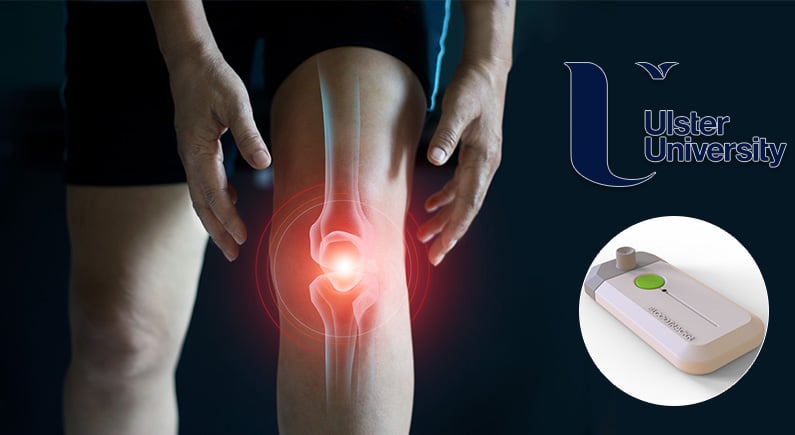
Researchers at Ulster University aim to help arthritis patients keep themselves well by using BloodTrackR, a device with the potential to detect the early signs of flare-up in the patients.
BloodTrackR is a new blood collection device with the potential to allow rheumatoid arthritis patients to detect the first signs of a flare-up of their condition at home. The researchers’ principal goal for this new device is that, alongside being reliable and robust in its design and execution, it will be highly user-friendly.
“Trying to get the right medicine to the right patient at the right time” is how Dr David Gibson, principal investigator on this project, explained the fundamental philosophy behind this work. Dr Gibson is also the research group lead of the Personalised Medicine Centre and senior lecturer at the School of Biomedical Sciences at Ulster University. The biochemist has been involved in arthritis research for over 15 years.
Rheumatoid Arthritis and A Chance at Remote Arthritis Management
Rheumatoid arthritis is a systemic and chronic inflammatory disease characterized by inflammation of the synovium of any joint, including both small and large joints, leading to the destruction of bones and cartilage. This in turn may cause significant disability and even permanent loss of function.
Rheumatoid arthritis is the most common inflammatory rheumatic disease, and the incidence increases with age. According to research by Matthias Schneider and Klaus Krüger, arthritis has a prevalence of 0.5% to 0.8% in the adult population. It is the leading cause of disability in Ireland and the UK.
It is a painful condition that is characterised by stiff and swollen joints which, at times, can significantly worsen — a state referred to as a flare-up. Flare-ups are more frequent when a patient’s treatment isn’t effective, predisposing the patient to a permanent disability or heart disease. Doctors, therefore, need to be able to identify these flares on time to prevent these complications. However, there are no fully tested options available to safely and reliably collect blood samples to monitor these flare-ups when a person is at home.
With BloodTrackR, there is the potential to monitor the condition while the patient is in the comfort of their home and also adjust their treatment remotely. This benefits both the healthcare service and the patient receiving the care.
The researchers, engaging patient groups, clinicians, medical scientists, med tech experts and the pharmaceutical industry, are working to test and develop the device through a series of three monthly user-experience workshops. After every 3 months, the patient gives feedback on a new iteration of the device and the new software. This two-year project seeks to develop a robust, user-friendly device from a regulatory standpoint, and an accompanying mobile app, which could then be used in healthcare or clinical trials. This is a patient-driven project, aiming to incorporate as much user feedback as possible.
The Regulatory Challenges in Healthcare
As with many new technologies, there are regulatory challenges. Since the effect of every new technology on patients is at the forefront of the criteria considered for approving the use of such technology, the process of developing a device and testing it on patients is highly scrutinized by regulatory bodies. If it passes, it will then have to be tested in the clinical environment where several questions will be asked, namely ‘does it improve health outcomes?’ and ‘is it cost-effective?
However, with about one-third of the world population affected by arthritis or other musculoskeletal disorders, the apparent potential positive impact of BloodTrackR makes it widely accepted by the affected population. Furthermore, what’s encouraging the researchers is the overwhelming positive feedback from people with arthritis.
Remote patient monitoring and the many benefits it offers became apparent as the COVID-19 crisis hit. The pandemic focused everybody’s attention on how to easily monitor long-term health conditions when people are away from the clinic and also alleviate pressure on the healthcare service.
In the past few months, the old medical practice model of doctor-to-patient has been witnessed to decrease in popularity. Instead, people living with arthritis are emerging as the experts of their own condition, allowing them to take a lead role in its management.
Take Part in Med-Tech World 2022
It is now estimated that the global digital health market will increase to around $640 billion by 2026. Through our expertise coupled with optimized networking, we will ensure that both investors and startups are on the ground floor of this health revolution. The event which is organized and curated alongside a team of doctors, attracts legislators and policymakers, medical professionals, and investors from across the world, addresses the opportunities and challenges driving this million-dollar forum.




